WHAT IS A HIGH ANKLE SPRAIN?
In the United States, about 2 million ankle sprains occur every year.1 Additionally, half of those ankle sprains occur during sport participation! If you have ever played sports, then you are probably familiar with the term “ankle sprain.” Traditional ankle sprains otherwise known as low ankle sprains tend to be the most common. However, one of the most severe types is called a “high ankle sprain.” Even though high ankle sprains are less common they are the most severe and difficult to return to sport participation because of location and pain level.
In a 2017 study of college athletes they found that high ankle sprains resulted in significant time away from sport participation.2 It takes approximately double the amount of time to return to a sport compared to low ankle sprains. Furthermore, the majority of high ankle sprains occurred with contact vs. the traditional low ankle sprain. These are significant findings in terms of contact sports such as football and ice hockey where the majority of high ankle sprains have occurred. Recently, players such as LeBron James of the NBA have suffered from a high ankle sprain when a player dove for the ball and struck his ankle. LeBron tried to return early from the sprain before the playoffs started and was not nearly the same player. He even stated that it took him three months to fully recover from the high ankle sprain during the off-season.
So what is a high ankle sprain?
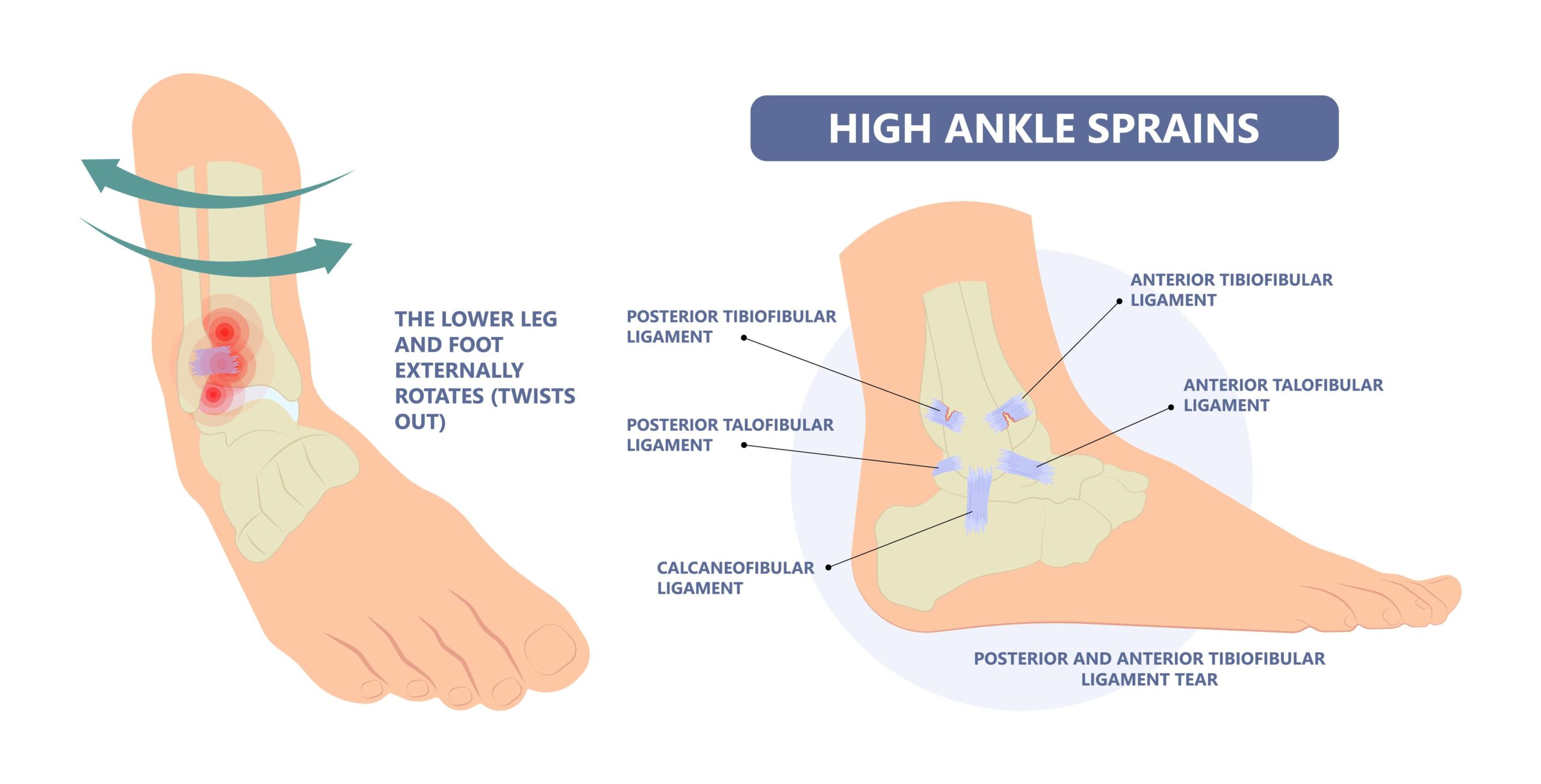
A high ankle sprain is when you damage the ligaments that connect the two lower leg bones the tibia (shin) and fibula (outside bone). The ligaments that connect the tibia and fibula together are known as syndesmosis and often a high ankle sprain is referred to as a syndesmotic injury. These are much thicker ligaments compared to the low ankle ligaments which makes the injury that much harder to come back from. The syndesmosis area provides a strong element of stability for the lower leg bones and when injured it can lead to instability issues.
How do high ankle sprains occur?
Typically, high ankle sprains occur from external rotation forces which causes the talus to rotate laterally which pushes the fibula away from the tibia causing separation of the high ankle joint. The ligaments that hold the tibia and fibula together are now stretched causing immediate pain. Often these injuries occur from contact such as someone hitting the outside portion of your ankle which forces your foot to dive in and externally rotate causing disruption between your lower leg bones. This has a huge impact on the recovery timeline because discomfort tends to linger compared to low ankle injuries. What becomes most difficult is your ability to cut, jump and land after a high ankle sprain. The syndesmosis area absorbs a lot of force transmission when your foot hits the ground. How is it different from other ankle sprains?
There are two common types of ankle sprains
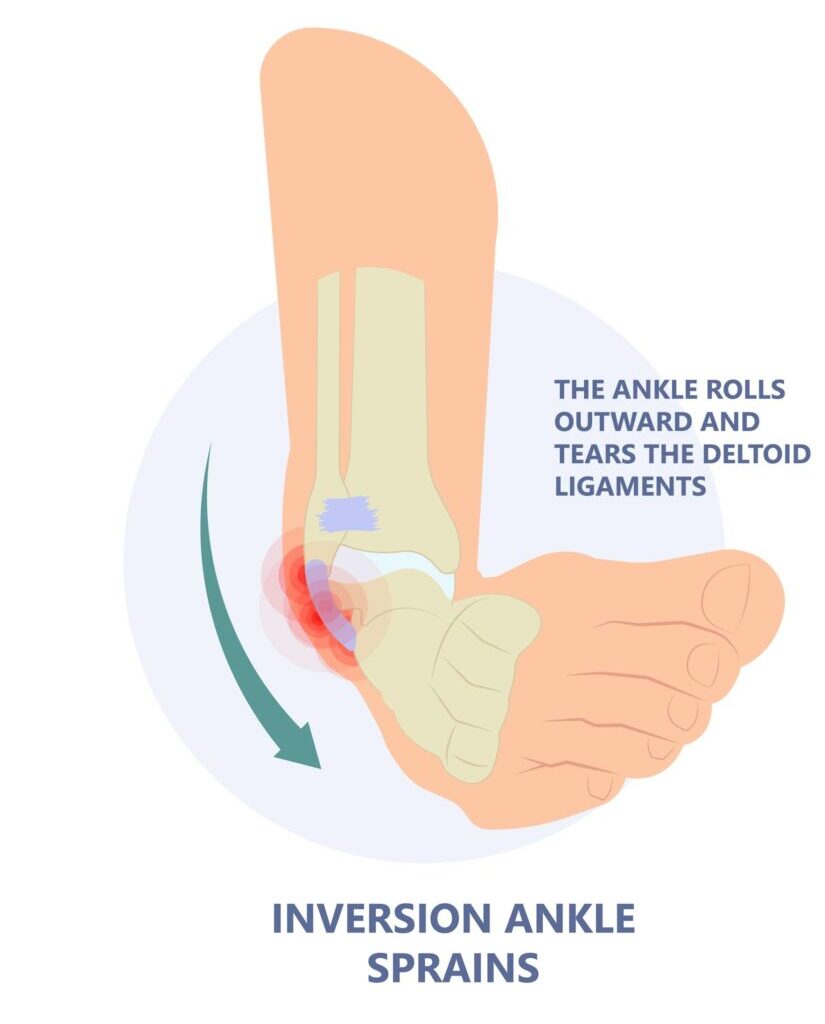
- Inversion ankle sprain: This is the most frequent type of ankle sprain which occurs when your foot turns inward. This will result in an overstretch of the lateral ligaments of the ankle
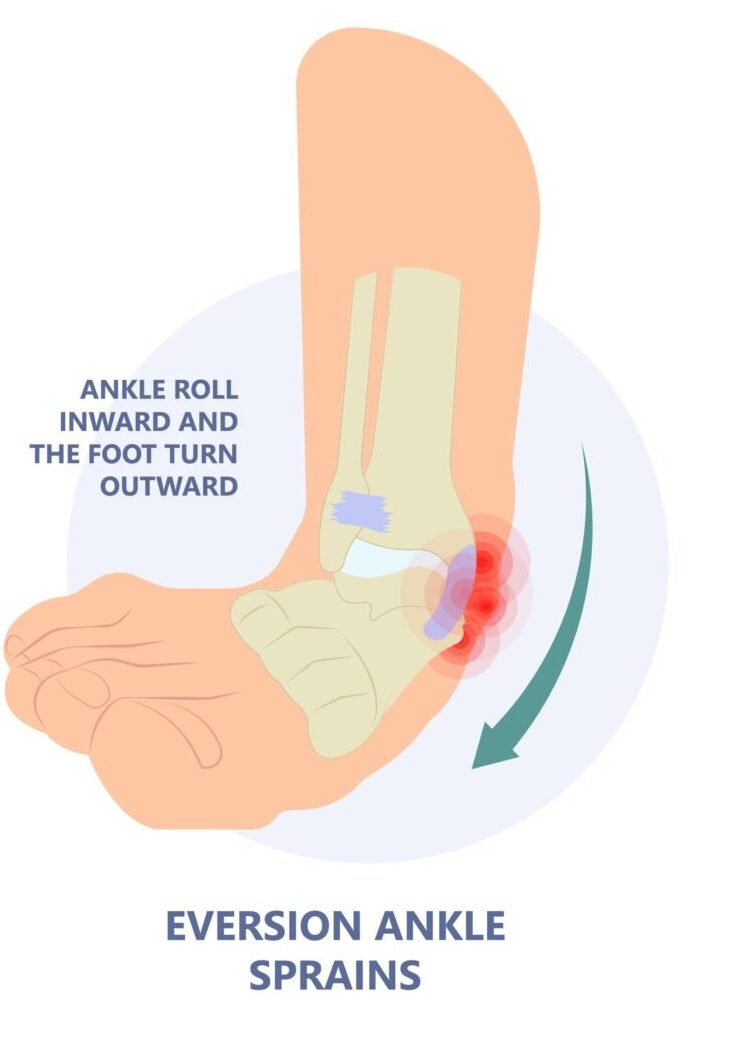
- Eversion ankle sprain: This is the less frequent type of ankle sprain which occurs when your foot turns outward. This will result in an overstretch of the medial ligaments of the ankle.
3 main reasons high ankle sprains are different than a low ankle sprain
- It typically occurs with contact which forces a strong ligament (syndesmosis) to separate from tibia and fibula.
- Recovery is usually twice as long as low ankle sprain because of pain and impact to the lower leg bones making it difficult to return to cutting, jumping and landing.
- It’s not a type of ankle sprain that you can just tape up and play because of the importance of the syndesmosis area to resist rotational and translational forces.
3 ways to reduce risk for high ankle sprains
- Protection: Using an ankle brace with rigid guards like the A2-DX can help reduce severity of a high ankle sprain or reduce impact of contact from another player.
- Train: Specific mobility and stability strengthening exercises can reduce the risk of a high ankle sprain.
- Improve balance/proprioception: A program built around proprioception can increase awareness of the brain to perceive where your body is positioned.
Playing sports at a high level puts you at risk for lower extremity injuries such as high ankle sprains. With ankle sprains being one of the most common types of injuries that occur with participation in sports protecting the joint would be a wise decision. Adding a layer of protection can reduce ankle sprains, limit severity of injury, and increase your availability to your team. Stephen Curry and Trae Young have been early adopters of the Zamst A2-DX ankle brace which has really helped their availability on the court. They are true believers of adding a layer of protection and reducing their risk for injuries. If you are worried about lack of mobility while wearing ankle braces look at Stephen Curry and Trae Young who are two of the most elusive point guards in the NBA.

Learn more about WHY TRAE YOUNG USES THE ZAMST A2-DX and about the entire Zamst ankle brace lineup.
ABOUT THE AUTHOR
Dr. EVAN JEFFRIES is a physical therapist with a Doctorate in Physical Therapy (DPT) from the University of St. Augustine for Health Sciences. He is also the owner of Evolving Motion and has vast knowledge of the musculoskeletal system and has treated many orthopedic conditions by bringing a proactive approach to healthcare and lifestyle. Recently he has also been active on social media as an injury analyst mainly in related to injuries NBA players have sustained. Evan can be followed on his social media accounts.
- Herzog MH, Kerr ZY, Marshall SW, Wikstrom EA. Epidemiology of Ankle Sprains andChronic Ankle Instability. J Athl Train. 2019 June; 54(6): 603-610.
- Mauntel TM, Wikstrom EA, Roos KG, Djoko A, Dompier TP, Kerr ZY. The Epidemiology of High Ankle Sprains in National Collegiate Athletic Association Sports. J Sports Med. 2017 Jul;45(9):2156-2163.






